- Shaping Innovative Products
- Unmet Needs & Clinical Insight
- Concept & Usability Testing
- Evaluating Market Opportunities
- Market Assessment & Market Sizing
- Buying Process, Procurement & Patient Flow Research
- Driving Commercial Success
- Value Proposition & Messaging Research
- Pricing Research & Pricing Strategy
- Launch & Portfolio Strategy
- Post-Market Surveys & Real-World Evidence
Switzerland (Head Quarters)
IDR Medical Switzerland
Austrasse 95, CH-4051 Basel, Switzerland
T:
+41 (0) 61 535 1109
UK
IDR Medical UK
Unit 104 Eagle Tower, Eagle Tower
Montpellier Drive, Cheltenham, GL50 1TA
T:
+44 (0) 1242 696 790
USA
IDR Medical North America
225 Franklin Street, 26th Floor
Boston, Massachusetts 02110, USA
T:
+1 (0) 617.275.4465

The German Hospital Landscape
Read this blog to learn more about the German hospital system and landscape, including how it is funded, structured, what its future looks like and more.
The German Hospital Landscape
Germany has twice as many intensive care units per capita as France, and almost four times as many as Italy or Spain.
Last year, a report published by an independent health economist, Bertelsmann Stiftung, suggested that Germany had “too many hospitals,” and recommended the mass closure of hospitals, prioritising quality of care over quantity.[1]
However, Germany’s management of the COVID-19 pandemic is primarily down to the amount of resource they have.
On the other hand, countries like Italy had their healthcare system pushed to the limit due to a shortage of hospital beds and ventilators. Therefore, the debate regarding mass hospital closure is ongoing.
In this month’s blog, we explore the German hospital system and landscape; how it is funded, structured, and what it's future looks like.
Organisation and delivery of inpatient care
Inpatient care is primarily delivered in acute hospitals and is available to all patients, regardless of whether they have statutory or private health insurance.
Rehabilitation facilities are also a form of inpatient care. Their main practise is to provide treatment to help manage patients’ physical condition following an accident or serious illness.
There are about 1,914[2] hospitals in Germany. Most of these are public (including some large university hospitals) and have less than 500 beds.
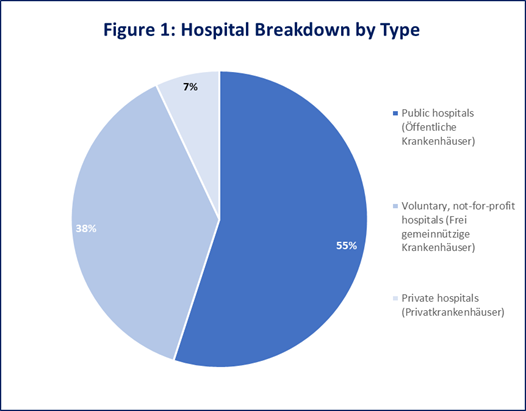 Figure 1 - Graph shows breakdown of hospitals by type.[3]
Figure 1 - Graph shows breakdown of hospitals by type.[3]
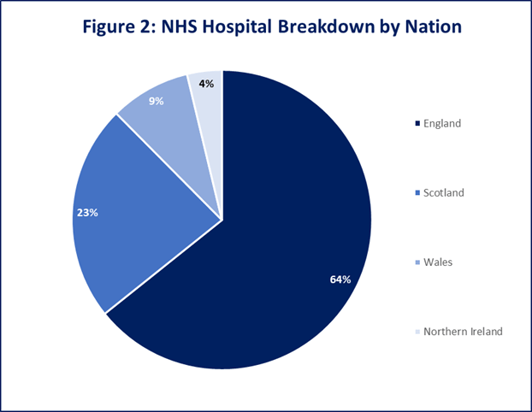 Figure 2 – Graph shows breakdown of hospitals by number of beds.[4]
Figure 2 – Graph shows breakdown of hospitals by number of beds.[4]
In Germany, hospitals are called Krankenhäuser and they differ by sponsorship. There are 3 main types that make up the German hospital system:
1. Public hospitals (Öffentliche Krankenhäuser)
These are run by the local and regional authorities.
2. Voluntary, non-profit hospitals (Frei gemeinnützige Krankenhäuser)
These are run by not-for-profit organisations, such as churches.
3. Private hospitals (Privatkrankenhäuser)
These offer inpatient care exclusively to patients with private insurance.
Hospitals also differ by service level. German state laws regulate 4 types of hospitals:
1. Basic service hospitals
These are small hospitals with up to 200 beds and 2-3 medical disciplines.
2. Regular service hospitals
These have up to 300 beds and 4-5 disciplines.
3. Central service hospitals
These have up to 500 beds and usually up to 8 disciplines.
4. Maximum care hospitals
These are big institutions with more than 1,000 beds. Most of these are university hospitals with a comprehensive spectrum of disciplines. They will also be responsible for research and training as well as treatment.
All levels offer state-of-the-art medical treatment. However, university clinics are not as accessible as central service hospitals as they offer treatment at the forefront of medical research.
Germany’s healthcare system is paid for by a combination of statutory and private health insurance, rooted in statutory regulations. Health insurance (gesetzliche Krankenversicherung – GKV) is compulsory for anyone whose gross earnings are below a fixed threshold.
Anyone who earns above the threshold can opt for private health insurance (private Krankenversicherung – PKV).
Unlike the UK, healthcare is primarily funded through the premiums paid by employees and employers. Premiums are income based so high-income earners help to subsidise low-income earners.
You can find out more about the reimbursement of medical devices in Germany in our blog, The Reimbursement Environment for Medical Devices in Germany.
Who is responsible for running the German healthcare system?
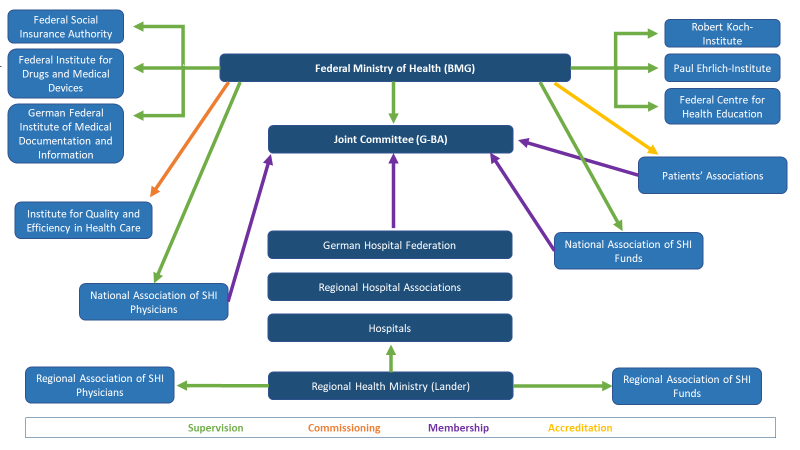 Figure 3 – Diagram showing the German Healthcare System[5]
Figure 3 – Diagram showing the German Healthcare System[5]
The Federal Ministry of Health (Bundesministerium für Gesundheit – BMG)
This is a cabinet-level ministry of the Federal Republic of Germany. It is the highest German federal government department responsible for health. Some of their responsibilities include[6]:
- maintaining the efficiency of statutory and long-term care insurance systems
- maintaining and enhancing the quality of the healthcare system
- establishing guidelines for the manufacture, clinical trial, approval, distribution channels and monitoring of medicines and medical devices
Overall, they aim to improve the population’s health. To that end, their specific areas of interest are health, long-term care, and prevention.
“Health” involves the safeguarding and further development of statutory health insurance. In 2007, the ministry implemented a major reform which improved the quality and efficiency of the healthcare system.
Furthermore, a 2008 reform saw a range of tangible improvements to long-term care; e.g., patients now have a legal claim to long-term counselling.[7]
Prevention is becoming increasingly important. The ministry has a range of successful initiatives in this area, for example “Life has weight” (a campaign for tackling eating disorders).
They are also responsible for outlining administrative guidelines to be implemented by self-governing bodies. There are a range of other healthcare institutions that the Federal Ministry of Health supervises and commissions (see figure 3).
For example, the Paul Ehrlich Institute which is involved in the approval of vaccines, and The Federal Institute for Drugs and Medical Devices, whose area of responsibility is the approval of pharmaceuticals. The most notable committee that the BMG overseas is the Federal Joint Committee.
The Federal Joint Committee (Der Gemeinsame Bundesausschuss - G-BA)
This is the highest decision-making body in the healthcare system. Made up of a range of representatives including dentists, psychologists, insurance providers, hospitals, and patients. Amongst other things, The Federal Joint Committee is responsible for[8]:
- defining which medical procedures will be covered by statutory insurance (and under which form the cover will be provided)
- quality assurance, carried out alongside The Institute for Quality and Efficiency in Healthcare (Institut für Qualität und Wirtschaftlichkeit im Gesundheitswesen – IQWiG) and other institutions
The German Hospital Federation (Deutsche Krankenhausgesellschaft – DKG)
This organisation represents a range of organisations responsible for running hospitals, including cities, not-for-profit associations, and private sponsors.
Understanding who is responsible for the German hospital system and landscape is complicated, there are various committee/associations all tasked with looking after different areas.
However, there is no doubt that the system is efficient, which is part of the reason why it was so successful during the COVID-19 pandemic.
Over the coming years we will find out if and how the German healthcare system will be re-structured.
If the report by Bertelsmann Stiftung is put into practise and hospital numbers are reduced, or whether The Federal Ministry of Health will heed the lessons learned during COVID and keep the structure the same.
Looking to conduct medical market research in Germany?
As an international healthcare consultancy, we have extensive experience conducting research in Germany and other countries across the globe, and can help you access the right stakeholders for your next market research project.
If you would like an initial telephone discussion, or an online meeting to understand how we can help your device take market share, please contact us today.
References
[1] Coronavirus crisis rekindles hospital debate in Germany | Business | Economy and finance news from a German perspective | DW | 21.04.2020
[2] Hospital statistics - basic data of hospitals and preventive or rehabilitation institutions, Federal Statistical Office, Bonn branc, 2019 Ad hoc table (gbe-bund.de)
[3] Germany: German hospitals, An overview of the hospital system in Germany, There are about 2000 acute care (justlanded.com)
[4] Beds set up and full capacity in hospitals (number), 2019 Hospitals Beds and full forces, e.g. by size class (gbe-bund.de)
[5] The Federal Ministry of Health - Bundesgesundheitsministerium
[6] EnWik > Federal Ministry of Health (Germany)
[7] Health, prevention, and long-term care in Germany (openaccessgovernment.org)
[8] Healthcare In Germany: The German Healthcare System - Welcome Center Germany (welcome-center-germany.com)

